A future free of dementia
An estimated 47.5 million people live with dementia worldwide, and by 2050 this figure is set to rise to 135 million*. A progressive disease that currently has no cure, dementia places a huge burden on families, carers and health systems. However, all this could change. Edit meets the inspiring individuals who, through their research, study participation and charity work, are improving treatment and reducing dementia risk.

Today, the total estimated annual global cost of dementia is $818 billion, and it will become a trillion-dollar disease by 2018. If dementia care were a country, it would be the world’s 18th largest economy.*
These figures make startling reading. But for those who have been affected by dementia, for those who have found it so rudely encroaching on their family life, there is almost always a number that matters more than any other: one. One mother, one father, one spouse, one friend. One mind that is slowly corroded, one personality so cruelly changed.
Yet in the face of this devastation, there is a renewed sense of hope. A radical movement aims to change both our perception and management of dementia, so that it is no longer feared as an inevitable condition of older people.
Globally, efforts have begun to challenge that long-held view, empowering young people to take control of their brain health and protect it decades before any symptoms appear. By tackling dementia risk in mid-life, and developing new treatments that knock out the earliest signs of disease, the goal is to rid the world of this illness.
Here four people who are making a real difference to the way we perceive and manage dementia share their knowledge, experiences and hopes for the future.
Craig Ritchie

Co-Director of the Centre for Dementia Prevention at the University and lead researcher for the European Prevention of Alzheimer’s Dementia (EPAD) project
Dementia is a term used to define a group of conditions that affect thinking and behaviour. They usually start in late life but research is now suggesting that the diseases that lead to dementia actually may start in people in mid-life. One of the major challenges we face in current dementia research is to approximate what happens inside the brain of people with the earliest signs of disease many years before symptoms develop. Historically, our analysis of the actual disease has had to take place in people who have died but this can only give us limited information about the disease processes themselves that led to dementia and, crucially, the timeline of biological events that lead to its development.
The approach to date for predicting how biological patterns affect clinical symptoms has been relatively simplistic. It can be thought of through an analogy with weather forecasting. Decades ago we tried to predict the weather with only limited amounts of information drawing conclusions from, for example, the ‘red sky at night’ to try and see patterns that may help us say what will happen to the weather in the morning. It wasn’t until we developed the technology to track and analyse meteorological data on a vast, global scale that we were able to predict future weather patterns with any accuracy hours, days and now even weeks ahead.
We need to approach dementia and the underlying neurodegenerative diseases in the same way. By identifying the earliest patterns of disease which predict or ‘forecast’ dementia we hope to develop treatments that will knock these early disease processes down before they go on to cause further problems. This approach has worked well with almost every other major, chronic disease, and particularly in cancer, where we have become skilled at diagnosing tumours early and eradicating them before they grow and spread.
Those are the questions that the European Prevention of Alzheimer’s Dementia (EPAD) and PREVENT Dementia projects, both of which are led from the University, aim to answer. Our goal is to gather comprehensive health, biological and risk factor data from thousands of volunteers in their middle age and early old age, and follow them up over time to see which risk factors have the greatest impact on brain health and how changes in the biology of the brain relate to clinical symptoms.
In the same way that you would use barometers, thermometers, and hygrometers to measure the weather, we now have advanced technology to analyse accurately what is going on inside the brain. For instance, we use imaging techniques like diffusion tensor imaging to see brain structure in detail. We have worked with neuropsychology experts from all over the world to develop improved cognitive testing that allows us to home in on specific areas of the brain, like the hippocampus, which is often the first to be affected in dementia.
As we gather all this information, we can start to identify patterns that will help us predict the disease process in the population at large and, ultimately, we hope to be able to give any individual an accurate prediction of their dementia risk, with practical personalised interventions that can reduce it.
With the right investment, scientific expertise and political will, it may well be possible to all but eradicate dementia in our children’s lifetimes.
We already have hundreds of people enrolled in the PREVENT Dementia project, and recently opened new sites at the Universities of Oxford and Cambridge – in fact we have more volunteers than we are currently funded to recruit, which is an amazing testament to the motivation and generosity of people who have in one way or another been impacted by this disease. EPAD will have at least 6,000 participants from across Europe by the end of this decade and we plan to begin trials of interventions to prevent dementia in that cohort in 2018.
These projects represent major steps on this journey, and now we need people to come along with us. We need volunteers to join our studies, we need donors to support us over the long term, and we need governments and industry partners to deliver public health campaigns so we are all empowered to take control of our brain health. If we can do it for cancer and heart disease, there is no reason we can’t do it for dementia, and in just the same way, the rewards could be staggering. With the right investment, scientific expertise and political will, it may well be possible to all but eradicate dementia in our children’s lifetimes.
Centre for Dementia Prevention
Video
Professor Craig Ritchie talks about the Engage study on Join Dementia Research.
Adam Waldman
Chair of Neuroradiology at the University
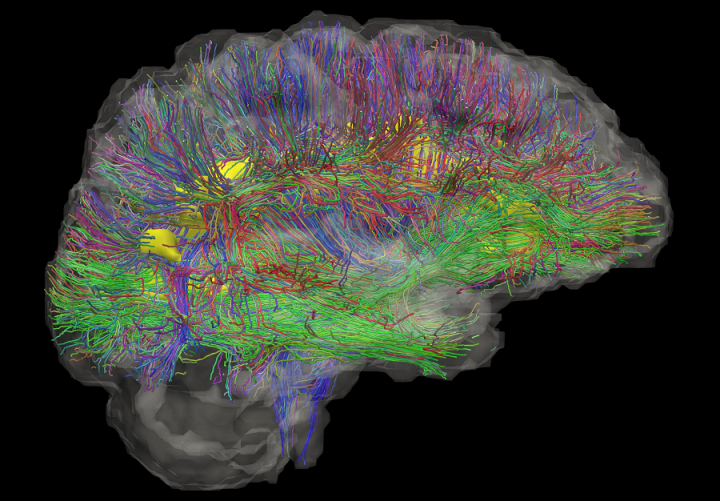
One of the reasons that imaging is so valuable is it allows us to look at the brain objectively, in a non-invasive way. With other diseases, you can biopsy the affected tissue, but with the brain, unless you have a very, very good reason to do so, that may cause more harm than good.
Today’s imaging capability gives us the potential to detect the earliest pathological changes that underlie dementia. That is important for two reasons: firstly, it helps us to diagnose early, which we know is key to tackling any major condition. Secondly, it may allow us to distinguish the particular type of dementia, which increases the likelihood of finding the right treatment.
We know that the brain changes decades before the symptoms of dementia appear. Evidence now suggests that as part of the disease cascade, two proteins build up in the brain – amyloid and tau. Together, these toxic proteins lead to neurodegeneration and ultimately cell death.
There are many important ways of measuring these brain changes, including analysing cerebral-spinal fluid through lumbar punctures and identifying those with genetic risk through blood tests. But imaging adds an important advantage – through PET and MRI scanning we can see where these proteins are building in the brain, and crucially how this changes over time. We can detect inflammation in brain tissue and measure any shrinkage, all of which are the hallmarks of this condition. And importantly, we can measure brain function, to determine what impact these biological changes have on cognitive ability.
In Edinburgh, we have superb imaging facilities as a result of huge investments in this area. It is staggering to see how the field has changed even in the past 10 years, and we are very fortunate to have not only the most advanced scanners, but also the expertise to develop the techniques that put them to greatest effect. We are positioned within an established clinical setting and that critical mass makes it possible to develop fantastic momentum. Edinburgh now has the largest group of neuroimaging experts in the UK and we have tremendous ambition in what we could achieve.
Centre for Clinical Brain Sciences
Julie Duffus
First participant recruited to EPAD

I got involved in dementia research because both of my parents had dementia. My mum died first, and then my dad a while after. Both of them had been involved with research in their lifetimes and I felt that now it was my turn. I signed up to the Join Dementia Research campaign, who matched me with the PREVENT Dementia research project in Edinburgh. A few months later I was contacted by Professor Ritchie who asked if I would be interested in becoming the first participant in Europe to join the EPAD study. I was excited by the prospect and felt very happy to get involved.
From my experience of caring for my parents, I know how dementia manifests itself at the end of life, and the issues you face in caring for a loved one with the disease. This isn’t a disease that just affects the individual, it changes your family completely. We couldn’t keep my Dad in his own home because he kept leaving the house at 5am in his pyjamas and being found by the police. It was just awful, both for him and our family around him. When someone with dementia dies it is like a double bereavement because you have already lost the person you love once, robbed of their personality by an, as yet, incurable disease.
EPAD is different from everything else I’ve heard about in dementia research because the emphasis is on middle age. We are not yet at the point of being able to predict a person’s risk in advance, and of giving them advice on how they could reduce it. If we could do that it would change everything.
Volunteering for the study has been a wonderful experience. I have found it fascinating. Although I have worried about different elements of the testing – I thought I would feel claustrophobic in the MRI scanner, for example – when the time came, I didn’t feel uncomfortable at all. The staff put me at ease and when you’re taking part in something that you feel is so important, you can’t let nerves get in your way.
As it’s a European project, one of the things I am most interested to find out is whether there are any geographical differences in what the research shows. You hear that the Mediterranean lifestyle is good for your health, so it will be good to see if that comes out in the data about dementia risks too.
Through my involvement in EPAD, I have become passionate about the need for this research. I know that I would rather get any other disease than dementia. We need to fix it, and hopefully, with projects like this, we are on our way. I hope that my contribution will in some way help us to find better ways of diagnosing the disease and potentially, one day, to prevent it.
Sally Magnusson

Alumna, TV presenter, writer and founder of dementia charity Playlist for Life
Dementia was something I had given very little thought to. Until it comes knocking at your own door you are not aware, and may be, in fact, profoundly ignorant, as I now realise I was. Gradually, over 12 years, it began to engulf my life. My mother was a very lively, smart, vivacious, gregarious person and watching the symptoms of what turned out to be Alzheimer’s and vascular dementia ravage her was very, very painful. It was also a very lonely experience, which is why I wrote my book, 'Where Memories Go: Why Dementia Changes Everything', to try and talk about this.
Stigma is like some sort of bacteria that feeds on silence, it feeds on people holding it inside and not sharing it, it feeds on shame. There has been a shame attached to dementia because families become wary of a loved one being in company in case they say something offensive, or do something silly. You’re trying to protect them and you’re also trying to protect that bit of yourself that just wants things to be normal.
All these things have conspired to keep dementia under the radar, and it remained there even while people were living longer and longer, and the numbers of those affected increased. By not talking about it, we as a society failed to put the social supports in place that were so badly needed.
We are much better at that now. We are talking about it more, governments are thinking about it more and we are getting a bit better at bringing to families and people with dementia the support they need. But there is still a long way to go and we have to work even harder at it, because this is a disease for everyone. There is not going to be a family in the land who will not be affected in one way or another. Nobody will be untouched by this.
My hope for the future is that you can get a diagnosis of dementia and not feel that your life is over. That you are able to continue living as full a life as possible, among people who understand what dementia is and what it isn’t. That you shouldn’t feel you can’t tell your friends or workmates because they will treat you differently.
I have read a lot of the research over the years and have seen many exciting things happening in mice and rats, but unfortunately when they have been rolled out in large, and expensive trials, they have not yet worked in human beings. That’s why I am so supportive of the work going on in Edinburgh right now. By gathering all of this information on what causes the disease in its very earliest stages, and differentiating between what could potentially be up to thousands of disease strains, there is a possibility that the game could be changed for generations to come.
My hope for the future is that you can get a diagnosis of dementia and not feel that your life is over.
My mother talked about feeling like she was on a long road, getting further and further away from herself. That feeling of detachment must be just the most frightening and lonely experience to have. Music can connect somebody to the person they feel themselves to be, and it can connect them to the loved ones who feel they have lost the ability to talk to them.
I set up the charity Playlist for Life to encourage families to offer personally meaningful music to those they love with dementia, as a means of helping to combat that isolation. It’s about connecting a person to themselves. My hope is that every single person in the country becomes aware that personal music can be a powerful tool that can alter mood for the better, help cognition and improve memory. I want the experience of dementia to be a happier one. All the evidence suggests that access to the soundtrack of their lives can keep bringing people back to themselves for a while, right to the end of their lives – and no drug can do that yet.
* World Alzheimer’s Report 2015 and 2016, Alzheimer’s Disease International.

