Themes
Primary care has great potential to deliver palliative care and end-of-life care. Five major and two cross-cutting themes of the work of this research group explore that potential.
All illnesses
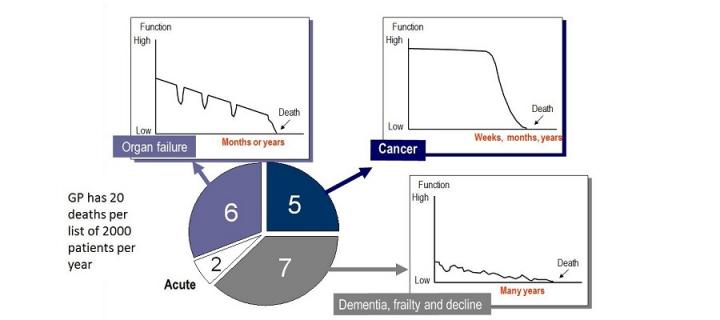
Identify and treat people with any and all life-threatening illnesses, taking palliative care beyond cancer from which only 25% of people now die.
All times
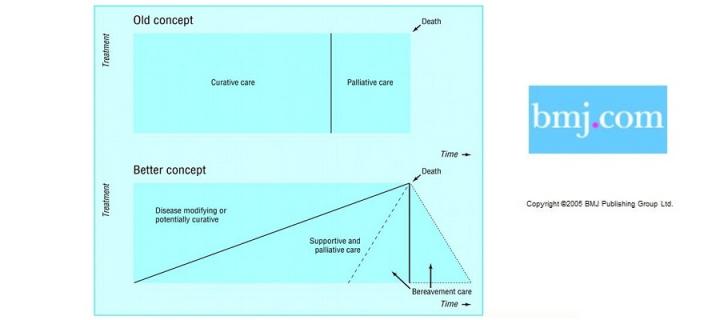
Help people earlier rather than later, not just in the very terminal stage but from diagnosis of a life-threatening illness.
All dimensions of need
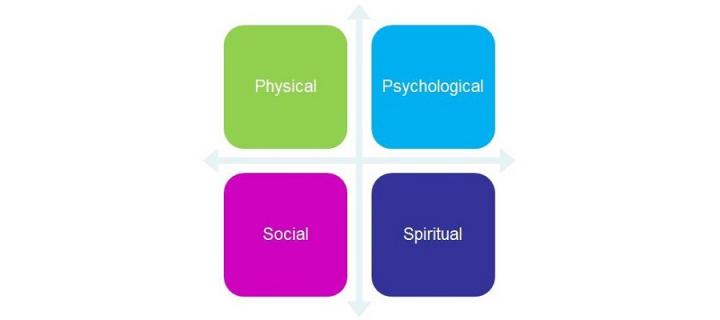
Care for all aspects of the person, all dimensions - physical, psychological, social and spiritual - as good general practitioners already do.
All settings

Quality palliative care can and must be delivered by generalists in hospitals, at home and in nursing homes to reach everyone. With training and innovative support from specialists, even complex chronic disease management can be provided in the community. Co-ordination and sharing of electronic patient records can facilitate this.
All nations

Make end-of-life care available for people in all nations, especially the poorer countries.
Carers
A cross-cutting theme of our work considers the needs of carers. There is an opportunity for primary care teams to support family carers in their time of care and subsequent bereavement; as family carers are frequently cared for by the same primary care practice.
Health Promoting Palliative Care
An approach developed in Australia and being adopted around the world that recognises the importance of community involvement and social attitudes to dying and death in the search for a 'good death for all'.

