BLOG SERIES - A lifelong journey with asthma | Dr Katherine Hickman
Dr Katherine Hickman is a GP, Vice-Chair of the Primary Care Respiratory Society, and Primary Care Lead for the National Asthma and COPD programme. In this final blog in the series she offers a thoughtful insight into the lifelong journey of living with asthma
When a patient is diagnosed with asthma they are starting on a journey. A journey that for the majority will last a lifetime. If that patient starts off on the wrong foot and travels down the wrong path it is unlikely to be a smooth one. They may feel alone, confused, scared and unsupported. The information they received at diagnosis may have been minimal and they leave with no idea on how to manage their asthma outside of the GP surgery or A&E. Equally, they may have been bombarded with untailored information, given leaflets, access to videos on inhaler technique, signposted to Asthma UK, the RightBreathe app and something called a Personal Asthma Action Plan (PAAP) that ‘is four times more likely to keep them out of hospital’ if they use it.
These resources may well have worked for the ‘perfect patient’ in a ‘perfect’ RCT under ‘perfect’ conditions. We are not, though, working or living under perfect conditions; we are living in the real world and we are trying to do our best. Pre Covid-19 we were under immense pressure and the pandemic has only exacerbated this problem. It has exposed services that were already at breaking point and also highlighted the inequalities of our patients. We are treating patients, up and down the country, with vastly different health needs, ideas, beliefs, social and economic circumstances.
For some patients, before they make contact with a Healthcare Professional (HCP), they will have developed deep seated beliefs around asthma- beliefs based on their own lived experience or from friends and family. The initial consultation is so important. If a patient sees a HCP who lacks specific knowledge on how to manage asthma, is ignorant of the resources available and is not confident filling out a PAAP this will only compound the problem. If they don’t also address the patient’s beliefs from the outset it potentially creates a perfect storm.
Maslow's hierarchy of needs is a theory of motivation which states that five categories of human needs dictate an individual's behaviour. If we apply this to asthma care and take inspiration from our series of blogs it might look something like this:
Patients
Basic Needs
- Physiological needs: Every patient knows HOW to take their inhaler and WHY they are taking it
- Safety needs: Access to resources and an Easy Read PAAP in their own language and they know WHAT to do in an emergency
Psychological needs
- Belongingness and love need: Supported self-management from their asthma ‘team’ and if they can’t get an appointment with their GP or nurse they can go to their pharmacy or ‘wellbeing centre’.
- Esteem needs: Learn to celebrate all wins - not perfect adherence but optimal thus reducing their over-reliance on SABA
Self-fulfilment needs
- Self-actualization: Realise their potential and live a life where they are in control of their asthma not the other way round.
Asthma Team
Basic Needs
- Physiological needs: Basic level of education/coaching on how to make a diagnosis of asthma and start them on their journey
- Safety needs: Through education and coaching know how to manage an asthma attack and fill out a PAAP. Provide proactive care rather than reactive that suits both parties safely via face to face, text message, video consultation or group consultations.
Psychological needs
- Belongingness and love needs: Work within an integrated care system with supportive colleagues who are familiar with the local population
- Esteem needs: Celebrate our successes, our improvements, our small, even tiny, changes and how far we have come and not how far we have to go.
Self-fulfilment needs
- Self-actualization: Realise their potential to provide great asthma care to their patients and the transformative effect it can have.
Living with asthma is rarely a smooth journey. I believe though, it can and should be, a lot smoother for our patients. It is our duty of care to ensure it is as smooth a journey as possible. We must minimise the speed bumps and the potholes, steer them away from the cliff edge, keep them on the right path and guide or carry them when they need us most. In Alastair JA Duff’s blog he talked about the importance of supporting patients to accept their asthma; ensuring that they are not burdened by it, like trying to keep a beach ball underwater and never knowing when it is going to pop up unexpectedly. How about we work with our patients to deflate the beach ball, put it in their rucksack and start them on their journey of a life living with asthma? And if you get basic care right you may just end up transforming a patient’s life and receiving an email like this one:
Good afternoon Dr Hickman. Many years ago you refused my repeat prescription request for my Asthma inhalers. You told me to make an appointment to see you. I wasn’t very happy. I was a fit chap, trained every day and couldn’t see the point. I explained that I take a puff on my blue inhaler before training, can train to the extreme and I had everything under control. You explained that I wasn’t in control and explained why. Since that first chat, I can’t remember the last time I used my blue inhaler. I thought I was doing ace, you challenged that, and I am better now than I was at 20 years of age. I’m now 53. In short, you changed my life. You taught me to better manage my Asthma, thank you so much.
Watch the webinar again
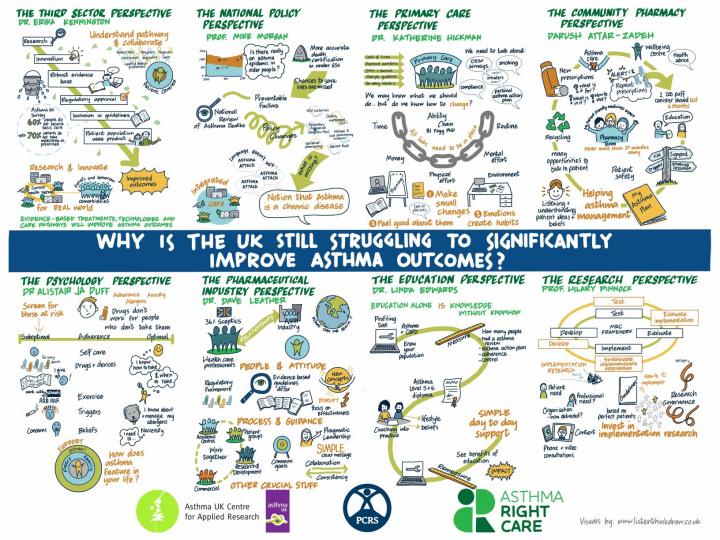
Watch our webinar ‘Why is the UK still struggling to significantly improve asthma outcomes?’ hosted in association with the Primary Care Respiratory Society.
Image credit: www.listenthinkdraw.co.uk

