Global health research needs gravity shift to deliver impact
A successful Africa-led global health research programme, contributing to World Health Organisation (WHO) policy development, has shared the key to its success and is calling for a shift in the centre of gravity of health research, designed to benefit developing countries.
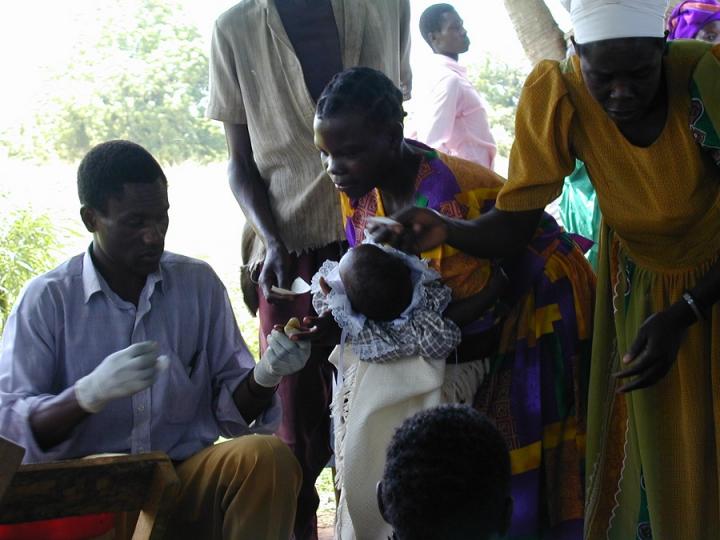
A case study of the TIBA (Tackling Infections to Benefit Africa) partnership highlights the need for cultural change in the ways western funders and researchers work with developing country researchers, stakeholders and affected communities on health challenges.
TIBA, a global health research and delivery partnership focused on strengthening health systems to tackle neglected tropical diseases, malaria and emerging infections in Africa, is challenging traditional approaches to health research.
TIBA has published the lessons that underpin its success and led to impact in multiple African countries - informing national and international policy on neglected tropical diseases.
Its emphasis on equitable partnerships created governance and management processes that enabled African partner institutions to define the agenda and direction of their own research.
Global Health Research Challenges
International research programmes designed to improve health in developing countries are often funded and led by international partners, including richer western countries.
Traditional approaches taken by western funders and researchers can lead to bias and inequalities that limit the success of international development research programmes and interventions.
Researchers and funders can be guilty of a series of common pitfalls such as conducting research that is not relevant to the local context or to local communities, meaning there is no buy-in or uptake.
Limiting the role of developing country partners to data gathering or failing to properly engage with stakeholders, including partners implementing the changes, can also hamper success.
Unequal power dynamics can result in western partners being the primary beneficiaries, including authorship positions in papers, limiting career progression for developing country researchers.
Equitable Partnerships
Attempts to tackle these issues individually often lead to temporary or unsustainable improvements focused on the symptoms rather than causes, which lie at a deeper cultural or management level.
To tackle these challenges TIBA, a partnership between the University of Edinburgh and nine African partner institutions, developed an equitable model of research and capacity building.
In just four years, with a budget of £7 million, TIBA demonstrates that health research for Africa thrives when the agenda and priorities are set in Africa, by Africans, and the work is done in Africa.
TIBA focused on shifting the centre of gravity of health research to African partners - with local agency, local control of the majority of resources, local prioritisation of research and impact areas.
Impact
All TIBA partners benefited from access to training and capacity-building opportunities and the majority of publications have Africa-based first and/or last authors.
The research improved the evidence base on African health systems and infectious diseases - contributing to international policy guidelines including the WHO NTD Roadmap, as well as national policy briefs on the deworming of adolescent girls and women.
The approach also enabled TIBA partners to pivot their expertise to COVID-19, generating evidence that informed the response of both national governments and international agencies.
TIBA researchers were involved in variant detection and tracking that contributed to global health security, conducted research on diagnostics and the protection of healthcare workers and advised on the provision of medical oxygen.
TIBA remains a leading example of the real-life transformative impact academic researchers can make on health and healthcare through multisector, interdisciplinary, and inclusive engagement.
Thanks to the outstanding work of our African partners, TIBA has delivered excellent science and had a direct impact on health security in Africa.
The case study has been published in BMJ Global Health. TIBA’s research was initially funded by National Institute for Health Research (NIHR).
TIBA involved researchers from partner institutions in Ghana, Sudan, Rwanda, Uganda, Kenya, Tanzania, Zimbabwe, Botswana, South Africa and the UK. Fifteen other African countries have participated in TIBA activities.


