Dr Gwo-tzer Ho
Research Theme in a Nutshell: Science to medicine: Inflammatory triggers to tissue repair in IBD.
Dr Gwo-tzer Ho
Reader / Honorary Consultant Gastroenterologist

- Centre for Inflammation Research
Contact details
- Work: +44 (0)131 242 6653
- Email: gho@ed.ac.uk
- Web: Academic Profile
Research Theme in a Nutshell:
Science to medicine: Inflammatory triggers to Tissue Repair in IBD
My research is focused on two main questions:
1. What are the molecular factors that drive and maintain the abnormal musocal inflammation in Crohn's Disease (CD) and Ulcerative Colitis (UC)?
2. How do we translate this understanding to develop new, and to improve current, medical treatments for CD and UC?
Group Members
- Dr Alex Cavanagh (Jean Shanks Pathological Society PhD)
- Dr Rebecca Hall (MUSIC MD Clinical Fellow)
- Mr Duncan Rutherford (CSO Clinical PhD Fellow)
- Dr David Wands (MiniMUSIC Paediatric MD Fellow)
- Dr Peter Cartildge (MUSIC MD Clinical Fellow)
- Mr Robert Whelan (MRC Precision Medicine PhD Fellow)
- Dr Gareth Rhys Jones (Wellcome Trust Intermediate Fellow and GI Consultant, Western General Hospital)
- Dr Rahul Kalla (NRS Fellow and GI Consultant, Royal Infirmary Edinburgh)
- Dr Claire Adams (ECAT PhD Fellow – 2nd supervisor with Dr Calum Bain)
- Miss Doireann Gordon (MRC iCASE Precision Medicine – 2nd supervisor with Professor Marc Vendrell)
- Phoebe Lau (Research Assistant)
Clinical Trials
- Miss Beena Poulose (Senior Research Nurse, Western General Hospital)
- Miss Athena Oddy (Research Nurse, Western General Hospital)
- Mrs Michelle Wilson (Research Associate, Royal Sick Children’s Hospital Edinburgh)
- Mrs Lisa Derr (Trial Manager for MARVEL and MiniMARVEL)
- Miss Katherine Lewis (Trial Support Officer)
Our Patient Public Involvement Team
- Mr Kris Gourlay (MUSIC)
- Miss Molly Halligan (MUSIC)
- Mr Jon Rysdale (MUSIC)
- Dr Kris McGuire (MARVEL)
- Dr Ola Helwak (MiniMARVEL)
Alumni
- Dr Shaun Chuah (2020-2022, MD University of Edinburgh)
- Dr Emily Thompson (2019-2022, PhD University of Edinburgh)
- Mr Broc Drury (2020-2022 Current EastBio PhD Student)
- Miss Rebecca Dimou (2022, MSc in Tissue Repair, University of Edinburgh)
- Dr Lena Fischer (Postdoctoral Scientist)
- Dr Ray Boyapati (2015-2018, MD University of Edinburgh)
- Dr Milly McAllister (2019-2022, Postdoctoral Scientist, now in University of Manchester)
- Dr William Brownlee (2020-2021, Postdoctoral Scientist)
- Mrs Jila Nazari (2019-2021, Data Manager)
Academic Awards
2016 – Fellow of Royal College of Physicians
2009 Medical Research Council Clinician Scientist Fellowship
2008 European Rising Star Award in Gastroenterology
2007 British Society of Gastroenterology CORE Research Prize
2005 European Crohn’s and Colitis Organisation (ECCO) Young Investigator Award
1997 – University of Glasgow (1st Class in Medicine)
I also lead the Edinburgh IBD Science Group, a diverse and cross-discipline group of immunologists, chemists, biologists, clinical trialists, clinicians and data scientists - with a shared vision to translate science to medicine. Please see GUT Research Unit.

Background
Crohn's disease (CD) and ulcerative colitis (UC) are common chronic inflammatory bowel diseases (IBD) with significant impact on morbidity, mortality and socio-economic costs. The global prevalence is increasing sharply with projected global disease burden of 20-30 million IBD cases by 2025. Present best therapies are based on the narrow principle of inhibiting downstream inflammatory pathways (eg, cytokines and inflammatory cell migration). Complete mucosal healing (total resolution of inflammation and restoration of full mucosal restitution) however, is achieved only in 50% in our best treatment. My work is focused on identifying and developing novel therapeutic approaches in IBD.
Research Overview
My overarching research aim is to translate new knowledge of immune and inflammatory mucosal mechanisms into new therapeutic approaches in IBD.
I work very closely with dedicated IBD clinicians, biologists, immunologists and drug development teams with a strong focus on direct studies on human IBD from laboratory scientific work to interventional human clinical trials. Major mechanistic themes are:
- Gut derived mucosal damage-associated molecular patterns (DAMPs)
- Mitochondrial dysfunction and ROS-signalling
- Metabolic programing of the mucosal immune response
- Active reparative mechanisms with novel targets focused on inflammatory monocytes-macrophage and T-cell trafficking.
Highlights of my research program:
1. MARVEL and miniMARVEL: From original scientific work (2009-2018), I have set up 2 UK multi-centre Phase 2b randomised controlled trial to investigate the use of mitochondrial antioxidants in adults and children with Ulcerative colitis (www.marvelstudy.uk). Here, I work very closely with David Wilson (Professor of Paediatric Gastroenterology, RHSC Edinburgh) to lead an ‘All-Ages’ IBD RCT.

2. Our MUSIC IBD project (www.musicstudy.uk) is a prospective longitudinal cohort study in Edinburgh, Glasgow and Dundee that aims to translate the clinical utility of mitochondrial ‘danger signals’ in IBD. Together with the cross-sectional GI-DAMPs study, we seek to study ~2000 participants to find new and simple tests to assess how the gut heals in IBD and potentially one day, replacing the need for colonoscopies.

3. Dr Shaun Chuah, current MD GI fellow, is investigating the role of blood cell-free DNA and its potential use as a ‘liquid biopsy’ and a mechanistic biomarker in IBD.
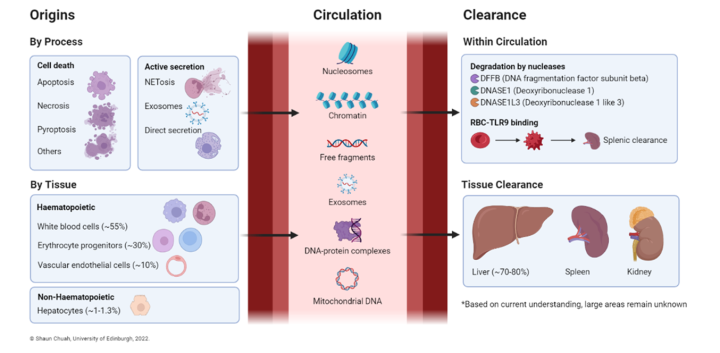
4. Dr Lena Fischer, our postdoctoral scientist is studying how fragments of DNA in the blood released during active inflammation in IBD can activate important immune cells that drives the development of IBD.
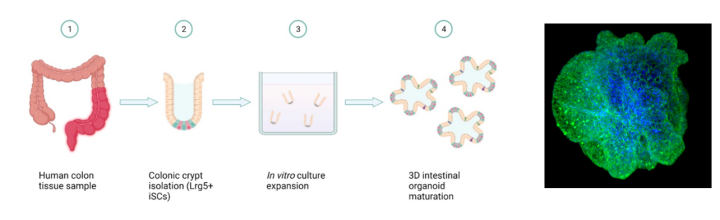
5. Mr Duncan Rutherford, our training surgeon (funded by the Chief Scientist Office) is growing ‘mini-guts’ or organoids on the dish from IBD gastrointestinal tract. His project is focused on the role of mitochondria in gut regeneration and how this can be used as another way to repair gut damage in IBD.
6. Dr Alex Cavanagh, our training pathologist (funded by Jean Shanks Pathological Society) is studying the role of Micro-fold cells (the gatekeeper of the gut lining) in Crohn’s disease and during the ageing process. M-cells are important in educating the gut immune system and we think is involved during the early stage of Crohn’s disease inflammation.

7. We have several human inter-related studies in trained immunity (Dr Rebecca Hall, GI fellow), immunometabolism (Dr Claire Adams, ECAT PhD Anaesthetics), NETosis (Mr Broc Drury) and specific translational projects into Granzyme A/B and oral microbiome (Miss Doireann Gordon and Mr Robert Whelan respectively) – funded by Wellcome and MRC.
8. With Professor Marc Vendrell (Translational Chemistry), we are collaborating synergistically to translate and bring to the clinic, new point of care optical technologies that can improve the way we track inflammation in IBD (www.dynafluors.co.uk/)
Find out more by watching our Let's Talk About Health public lecture from 2020:
- Video: Healing the damaged gut in inflammatory bowel diseases
- A recording of the Let's Talk About Health public lecture given on 19 February 2020, talking about the perspectives of a medical researcher, IBD patient and PhD student on current IBD research at the Centre for Inflammation Research.
- Video: IRR Discovery Series: Dr Thomas Fenton
- Dr Thomas Fenton, Visiting Scientist at the Centre for Inflammation Research, discusses a method he has developed which will give researchers a new way to analyse the intestinal immune system.
Dr Thomas Fenton, Visiting Scientist at the Centre for Inflammation Research (CIR), discusses a method he has developed which will give researchers a new way to analyse the intestinal immune system. Co-Lead for the Gut Research Unit at CIR, Dr Gwo-tzer Ho, also reflects on the discovery.
The following PDF provides a brief visual summary of this group’s current research.
You can view a full catalogue of graphical research summaries for each group in the Centre for Inflammation Research by visiting our Research page.
Biographical Overview
I trained in Medicine in Glasgow (MBChB 1997 and MRCP 2000), and moved to Edinburgh for my PhD with Jack Satsangi (2000-2003). I completed my specialty training in gastroenterology and internal medicine in Edinburgh (2003-2008) and was awarded an MRC Clinician Scientist Fellowship award (2009-2015) where I trained under Balfour Sartor in University of North Carolina, Chapel Hill, USA focusing on mucosal immunology in IBD. In 2018, I set up the Edinburgh IBD Science group and then the Gut Research Unit in CIR (2019).
With a strategic translational focus on human experimental work, my program supports a comprehensive portfolio of work across Scotland from basic discovery science to Phase 2 clinical trials in adults and children with IBD.
I continue to care for individuals with IBD working as an active consultant gastroenterologist at the Western General Hospital.
Current Committee/Editorial Positions
- I am Board member for the MRC Human Experimental Medicine and Developmental Pathway Funding Scheme (DPFS).
- I sit on the Crohn’s Colitis UK Medical Research Awards Board
- I am currently Chief Investigator to 3 UK multicentre human IBD studies
- I am the GI lead for 4th University of Edinburgh Medical School
- I am recent Associate Editor for Inflammation
- I co-lead MSc in Inflammation and Immunity with Dr Rodger Duffin and Professor Adriano Rossi
- I set up and lead the Scottish Translational Research (STAR) network, Edinburgh IBD Science and Gut Research Unit (GRU).
Collaborators
- Professor Kostas Gerasimidis, University of Glasgow
- Professor Balfour Sartor, University of North Carolina, USA
- Dr Laura Greaves, Newcastle Mitochondrial Unit
- Dr Mairi McLean, University of Dundee
- Dr Emily Findlay (University of Southampton)
- Dr Mahima Swarmy (University of Dundee)
Sources of Funding
- Crohn's Colitis UK
- Guts Charity UK
- Jon Moulton Foundation
- Genentech
- Wellcome Trust
- European Crohn's and Colitis Organisation (ECCO)
- Medical Research Society
More information on funding at Gwo-Tzer Ho's Research Explorer profile.
If you are interested in supporting our work by direct involvement, or funding our work on a charitable basis, please contact emma.watson@ed.ac.uk

